
From Tony Gentilcore
Lisa and I decided we were due for a little getaway. We’re back in my stomping grounds in central New York (specifically the Finger Lakes Region) to visit family and to partake in some long-anticipated vineyard exploring/wine tasting shenanigans.
Otherwise known as Tony drives Lisa to a shit-ton of wineries.
We’re having an amazing time with my family and couldn’t have asked for a more beautiful weekend
Knowing I was going to be away for a few days I planned ahead and scheduled an AMAZING guest post today by strength coaches Dan Hechler and James Darley. Today they’re going to discuss those silly altitude training masks that are all the rage nowadays that 1) people think actually work and/or 2) people use to pretend they’re Bane.
Like me.
Because I’m an asshat.
Nevertheless. It’s long. But well worth the read. Besides, if you can make it through a Bret Contreras post, you can make it through this. Trust me….;o)
Enjoy
Altitude Masks: Is There Science to Back Them Up?
The altitude-training mask — we’ve all seen them popping up across the country, from high-end performance facilities, to standard commercial gyms, and, of course, to our Instagram feeds. Athletes, weekend warriors, and bros are all donning this mask to achieve similar goals: increase their performance while simultaneously doing their best “Bane impression.” Bane jokes aside, the question is, do altitude-training masks actually increase performance, or do they slowly add to dysfunction?
Understanding the physiology behind the altitude-training mask is the first step to determining whether this tool is really worth implementing in our training.
While it may FEEL like it is making our workout harder, increased exertion alone does not necessarily mean it is actually OPTIMIZING our workout. By examining recent research on the mask, we can begin to gain a fuller understanding of its potential effectiveness.
Thus far, there has been little consideration of the body’s overuse of the accessory breathing muscles while wearing the mask. While the nitty gritty details of our body’s functioning may not be as captivating as this new altitude-training mask looks, it is well worth the discussion.
Hypoxic Training
To understand the creation and use of the altitude-training mask, it is beneficial to know the history and research behind hypoxic training.
Hypoxic training simply put is the practice of exercising, living in, or otherwise limiting relative oxygen availability to enhance athletic performance or acclimatize to altitude prior to an athletic event taking place at high-altitude (elevation above 5,000 feet above sea level).
In a high altitude environment, barometric pressure is decreased compared to sea level. While the percentage of oxygen in the molecules remain the same at around 20.9%, the decreased pressure causes less total molecules to be available as volume and pressure have an inverse relationship per Boyle’s Law.
In response, the human body over time adapts by the kidneys increasing erythropoietin (EPO) production, which stimulates red blood cell production in the red bone marrow, thus increasing RBC levels (Hematocrit). This allows for better muscle oxygenation.
History and Early Research
Before the 1968 Summer Olympic games in Mexico City (hosted at 7,350 feet above sea level!) the effects of altitude on elite athletes were understudied. This changed, since the Olympics saw the majority of elite endurance athletes underperform. Clearly, something was affecting their performance.
In an effort to prevent future negative surprises, scientists and researchers started to study the physiological changes that occurred in elite athletes when training and performing at high-altitudes.
Early studies conducted in the 1970s showed that training while living at altitude improved aerobic capacity (VO2 max) and improved performance at sea level. The issue with many of the early studies is that they failed to have a control group, which trained under the same conditions at sea level. And as we know, no control group = FAIL
Of course, this didn’t matter to strength coaches and elite level athletes. It was the height of the Cold War and national pride was at stake. When a tenth of a second can be the difference between placing and not placing, any advantage matters. So began the idea of hypoxic training and the creation of the United States Olympic Training Center in Colorado.
The Altitude-Training Mask & Research
Since the 1970s, our understanding of hypoxic training has advanced.
The most common form of hypoxic training is the live low-train high (LLTH) approach. This is when an elite athlete lives at sea level, but prior to an event, trains at altitude for a period of time determined by their coach.
This is the type of training that the altitude-training mask tries to mimic.
The altitude-training mask was created as a way to bring hypoxic training to the recreational athlete looking to improve their performance. After all, elite athletes do it to become better and gain a competitive edge, so why shouldn’t you? And best of all, at the super affordable price of $100 or less!
If you ask the altitude-training mask fanboys, they will tell you that the benefits are undeniable. You will experience increased lung capacity, oxygen efficiency, energy production, and physical stamina. Is there anything that it doesn’t do for you?
Now, does the research back up these bold claims?
The truth is that very few studies have been conducted on altitude-training masks. The one that is constantly used by companies that sell masks is a 2014 study by NAIT University.
In this study, 14 participants (8 male and 6 female) performed periodized high intensity interval training in a 5 week period while measuring V02 max utilizing the Rudolph valve maximal test and power output. One group used an altitude-training mask while the other used self contained breathing apparatus (SCBA) used by firefighters. There was no group performing the HIIT training without an altitude-training mask or SCBA. The study concluded that the altitude-training mask was equally effective as the SCBA. Since both power output and V02 max improved in both groups.
In essence, all the study proved is that HIIT improves your V02 max (earth shattering!) and that altitude-masks might be an item that can be used by fire departments to mimic wearing a SCBA.
It would be interesting to see, if using an altitude-training mask would be an effective and efficient way to train firefighters by strength coaches to simulate working fire conditions? I don’t have enough expertise with that population to comment, but would love to hear feedback!
Yet, what this study clearly does not do is support any of the bold claims made by the companies and altitude-mask advocates.
So, lets take a look at LLTH studies done without the use of a hypoxic training mask.
Several studies have looked at the LLTH approach utilizing normobaric hypoxia chambers with inconclusive determinations.
A 2005 study by Morton et al looked at short-term intermittent hypoxic training (4 weeks) in 16 trained athletes separated into two groups of 8. Both groups performed the same type of training program except one trained at sea level while the other trained at simulated altitude of 9,000 feet in a normobaric hypoxia chamber. The results showed that there were no advantages to training at altitude compared to sea level when looking at aerobic and anaerobic performance markers in such a short time frame.
A 2010 review by Vogt et al examined previous functional and muscular research done on LLTH training. They concluded that the performance data from previous research studies did not conclusively prove that hypoxic training lead to increased performance at sea level. Instead the evidence suggested that training at altitude made you better when performing at altitude. Imagine that! As a caveat, Vogt el al acknowledged that VO2 max markers and maximal power output data might not be sensitive enough to pick up slight performance enhancements in elite athletes.
A recent 2014 study by Richardson et al showed that simulated hypoxia sprint interval training conducted in a normobaric hypoxia chamber by 27 young participants did not improve V02 peak markers compared to sprint interval training done at sea level. Although both groups saw an improvement of V02 peak markers from sprint interval training.
The key conclusion is that LLTH training whether using a normobaric hypoxia chamber or altitude-training mask is most likely not going to improve the athletic performance in elite athletes.
In fact, using an altitude-training mask might actually be detrimental to athletic performance when you factor in breathing patterns and their importance to athletic endeavors.
Oh, and if you are a recreational athlete, don’t waste your money. You will avoid looking like a douche(tte) *we are equal opportunity here* and not to burst your bubble, but you don’t need an altitude-mask to help with your bicep curls and lat pulldown gainz.
PRI
To understand how certain breathing patterns affect performance and overall health, we first must review the inhalation process, and the Zone of Apposition, or the ZOA (oh yeah we’re going there).
NOTE FROM TG: HERE’s a post I wrote related on the topic of PRI and how, oftentimes, trainers tend to go too far down the rabbit hole when it’s not necessary.
During inhalation, the top of the diaphragm (dome) descends in a piston action, creating a negative pressure gradient in the thorax which drives air into the lungs.
During this process, the ribs rotate outward, the front of the spine pulls upward, and the bottom portion of the diaphragm helps pull the dome downward. To create more room for the dome to pull downward, the abdominal muscles relax, allowing the organs to move slightly. During vigorous activity, this abdominal activity is even more pronounced. With exhalation, the process is reversed.
When the ZOA is optimized, this process functions at a high efficiency rate.
Yet when the ZOA is suboptimal, and the dome cannot descend efficiently, the body may employ compensatory strategies. In one such strategy, the body relaxes abdominal musculature at a higher degree than normal to allow for proper thoraco-expansion.
However, overuse of this strategy can lead to decreased abdominal use during breathing and increased upper chest breathing, which will eventually shorten the diaphragm and hyperinflate the lungs.
You may be wondering, why the hell should I care about my ZOA and chest breathing? Well, having suboptimal ZOA and being a dominant chest breather will force you to heavily rely on the accessory breathing muscles, such as the scalenes, sternocleidomastoid, upper trapezius, pectoralis minor, and paraspinals.
During vigorous activity, inhalation is dramatically increased, becoming even more necessary than usual. We all know what it’s like to suck wind during conditioning or after a hard play. Now when we add a device to our training that makes it harder to breathe, what do you think our response will be: focusing on inhaling (the challenge due to the mask) or exhaling out that hard-fought air? Damn right, we’re inhaling longer than exhaling!
Now, let’s add that mask for 60 minutes of training, and we will begin to see the issues that start to pile up.
Our need to tap into the accessory inhalation muscles is heightened, and the associated dysfunctions come into play. When looking at these muscles’ individual functions, we begin to see the big picture unfold.
Scalenes

This muscle elevates the first and second rib cage, unilaterally flexing the head to the same side, while also bilaterally flexing forward (cervical flexion). Working at computers, cell phones, and desks puts us in a high degree of cervical flexion leading to a modern-day posture known as the “turtlehead.” Overuse of the Scalenes from excessive inhalation will only increase the neurological tone, continuously feeding this postural nightmare.
Sternocleidomastoid
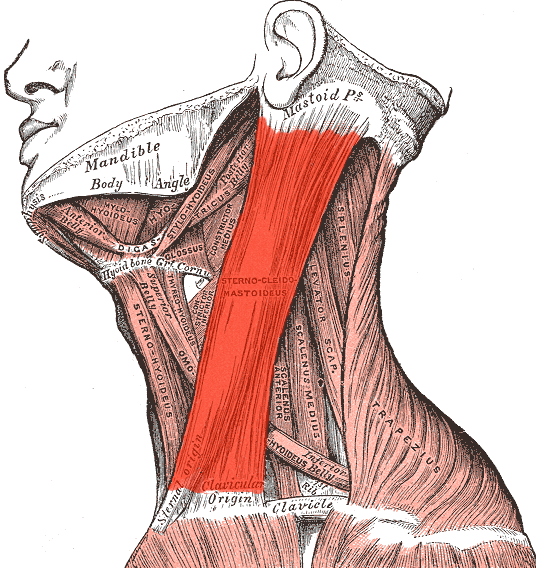
This muscle also elevates the first and second rib (see a pattern?), flexing and laterally rotating the head. Similar to the scalene, when used bilaterally, it causes cervical flexion. Overuse of the SCM can cause numerous health problems, most notably head or neck pain.
Upper Traps
This muscle assists in elevating the scapula and, in tandem with the serratus anterior and lower trapezius, contributes to upward rotation of the scapula. If overuse makes the upper trapezius too dominate, the ability to effectively execute overhead movements is greatly diminished.
Pectoralis Minor

This muscle stabilizes the scapula by pulling it forward, against the thoracic wall. In most (bad) programs, overuse results from excessive pushing movements and insufficient pulling. When the Pec Minor gets too tight from excessive pushing or computer use, it can cause rounded shoulders, leading to External Impingement. Combining overuse of the Pec Minor during mismanaged training programs with overreliance on it for inhalation during activity results in a recipe for disaster, and the oh-so-sexy Mr. Burns posture.
Erector Spinae

This muscle helps prevent flexion of the spine, keeping the body upright. Excessive use and neurological tone of the erector spinae adds to the dysfunction of excessive lumbar lordosis. The body has a natural curve (lordosis), but when the anterior core becomes over-lengthened (weak), lower back pain is often the result. One component of suboptimal ZOA is relaxed (weak) abdominals.
When we are putting in work during our training sessions, our ability to control and utilize our respiratory system as efficiently as possible is paramount. This control is one of the greatest advantages an athlete can possess. Adding a device that purposefully disrupts this ability during training teaches athletes different breathing compensatory patterns. As we just demonstrated, this compensatory strategy can lead to suboptimal ZOA, decreased anterior core function, increased muscle tone, and lower back pain. All these are recipes for injuries, and no one has ever won a game while on the bench.
Conclusion
Any respectable strength coach utilizes a risk versus reward criteria when programming for an athlete. If not, then you simply aren’t doing your job as a coach. When it comes to the altitude-mask, the overwhelming evidence shows that at best the device is ineffective and at worse, it might actually hinder your overall performance! I don’t know about you, but in this case, I think it is safe to say that the possible reward does not outweigh the risks of decreased performance and possible spike in injury occurrence due to increased breathing dysfunction.
Source: http://tonygentilcore.com/2015/08/altitude-training-masks-helpful-or-hyperbole/


